Effects of Stress on the Heart: #1 Essential Plan
Understanding How Stress Shapes Your Cardiovascular Health
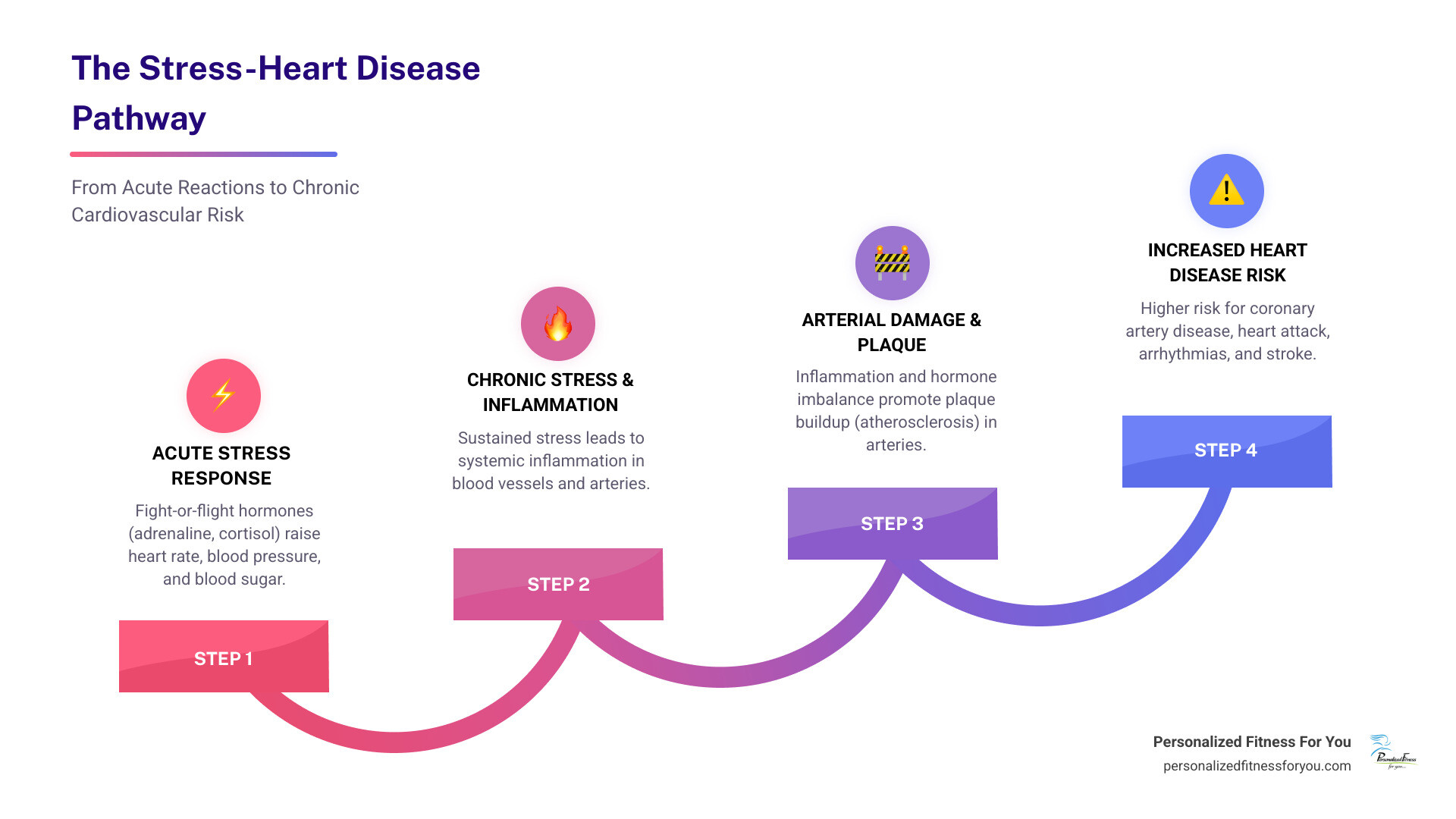
The effects of stress on the heart are both immediate and long-lasting, triggering a series of physical changes that can significantly impact your cardiovascular system. When you experience stress, your body releases hormones like adrenaline and cortisol, leading to immediate impacts like an elevated heart rate, increased blood pressure, blood vessel constriction, and heightened blood sugar levels. Over time, these responses can lead to serious long-term consequences, including chronic inflammation and arterial plaque buildup (atherosclerosis), which increases the risk of coronary artery disease. In some cases, severe stress can act as an acute trigger, rupturing existing plaque or causing coronary artery spasms that may lead to a heart attack. Stress also harms your heart through indirect pathways, encouraging habits like overeating, smoking, and sedentary behavior that compound cardiovascular risk. It can even lead to unique conditions like Takotsubo cardiomyopathy (broken heart syndrome) after intense emotional events, and it’s important to recognize that there are gender differences, with women being more prone to mental-stress-induced myocardial ischemia (reduced blood flow to the heart muscle).
The effects of stress on the heart are amplified by modern life, where two in three employees report significant work stress. For women in the Winona Lake and Warsaw area navigating demanding careers, family responsibilities, and the natural changes that come with active aging, understanding the connection between stress and heart health is essential. Rather than increasing anxiety, this guide offers a whole-istic perspective on the effects of stress on the heart to empower your wellness journey. You will learn about the immediate fight-or-flight response, the nature of chronic stress, unique stress-related heart conditions, and evidence-based strategies to protect your heart through movement, nutrition, sleep, and mindfulness.
I enjoy working with women to create a personalized program that takes a whole-istic approach. With Health coaching, we look at the heart and explore ways to reduce stress through a body, mind and spirit approach. Each of us is unque and our journeys are personal to us. Our bodies change with each season, and taking time to meet you where you are is important! A “cookie-cutter” fitness program generally doesn’t apply to each of us. Taking into account your health history is key to starting any program. Whether you are training for a race or interested in beginning a fitness program, I am here and ready when you are! Let’s move well, and be well!
The Body’s Alarm System: How Acute Stress Directly Impacts Your Heart
When we encounter a sudden threat or intense pressure, our bodies activate a primal “fight-or-flight” response, a rapid cascade of physiological changes designed for survival. This acute stress response directly impacts your heart by releasing a surge of powerful stress hormones.
The primary hormones involved are adrenaline (also known as epinephrine) and cortisol, along with norepinephrine. Adrenaline, often called the “fight or flight” hormone, dramatically increases mental alertness and causes your heart to beat faster and with greater force, significantly raising your blood pressure. Norepinephrine also contributes by elevating heart rate, releasing glucose into the bloodstream, and increasing blood flow to your muscles, preparing your body for immediate action. Concurrently, cortisol floods the bloodstream with glucose, providing quick energy, and causes blood vessels to constrict.
These immediate physiological changes can, in certain circumstances, trigger acute cardiac events. For individuals with underlying vulnerabilities, such as pre-existing plaque buildup in their arteries, a sudden surge of adrenaline and other stress hormones can contribute to plaque rupture. This rupture can then lead to the formation of a blood clot that blocks blood flow, resulting in a heart attack. Acute stress can also induce abnormal heart rhythms, known as arrhythmias, as the heart’s electrical system reacts to the heightened hormonal activity. Furthermore, these hormonal surges can cause temporary spikes in blood sugar and release cholesterol into the bloodstream, adding to the acute burden on your cardiovascular system. Understanding these rapid responses is particularly crucial for women in the Winona Lake and Warsaw area, as research suggests women can experience different physiological reactions to acute stress.
Ready to create a personalized plan that nurtures your spirit, mind, and body? Schedule your complimentary consultation with Joy today by visiting our contact page and start your journey toward a stronger, more resilient heart.
The Slow Burn: Unpacking the Long-Term Effects of Stress on the Heart
While acute stress delivers a powerful, immediate punch, chronic stress exerts a more insidious, long-term impact on your cardiovascular system, quietly eroding heart health over time. Chronic stress is defined as prolonged exposure to stressors, whether from demanding jobs, financial worries, or ongoing personal challenges. This sustained pressure keeps your body in a state of heightened alert, leading to a continuous overproduction of stress hormones like cortisol and adrenaline.
One of the most significant long-term effects of stress on the heart is its role in promoting systemic inflammation. When stress becomes chronic, it stimulates a low-grade inflammatory response throughout the body. This inflammation is a key factor in the development of endothelial dysfunction, a condition where the delicate inner lining of your blood vessels (the endothelium) becomes damaged and less able to perform its crucial functions, such as regulating blood flow and preventing clot formation. Over time, persistent inflammation and endothelial dysfunction contribute significantly to atherosclerosis, the hardening and narrowing of arteries due to plaque buildup. This plaque, a fatty deposit, can restrict blood flow to the heart, leading to coronary artery disease, a major precursor to heart attacks and strokes. Scientific research, including a 2017 study in The Lancet, has used brain imaging to link stress and cardiovascular disease episodes, showing connections between resting amygdalar activity (a brain region involved in fear and stress) and increased cardiovascular events.
These long-term effects mean that chronic stress is a major contributor to the development and progression of heart disease. Certain populations, such as those in high-stress professions or those experiencing social isolation, are particularly vulnerable. It’s also important to note that women are particularly prone to developing mental-stress-induced myocardial ischemia (MSIMI), a condition where stress reduces blood flow to the heart muscle. Findings from major studies like INTERHEART highlight that psychosocial risk factors, including chronic stress, are significantly associated with acute myocardial infarction. A personalized approach to fitness can help manage these long-term risks, whether you prefer in-person training or a virtual training program.
Beyond the Biology: Indirect Pathways and Unique Stress-Related Conditions
The effects of stress on the heart extend beyond direct physiological changes, encompassing a range of indirect pathways through which stress can subtly, yet powerfully, undermine your cardiovascular health. It also includes specific, stress-induced conditions that highlight the profound connection between our emotional state and heart function.
How Unhealthy Habits Fueled by Stress Harm Your Heart
One of the indirect effects of stress on the heart is the adoption of unhealthy coping mechanisms, which in turn create a detrimental ripple effect on our cardiovascular system. When we are under sustained pressure, we may unconsciously adopt behaviors that offer temporary comfort but ultimately harm our health.
Additionally, stress can significantly reduce our motivation for physical activity, leading to a more sedentary lifestyle. A lack of regular movement contributes to obesity, high blood pressure, and poor cardiovascular fitness. Disrupted sleep patterns are another common consequence of stress; chronic insomnia prevents the body from repairing itself and regulating vital functions, impacting everything from blood pressure to inflammation. Furthermore, some individuals may turn to increased alcohol consumption or smoking as ways to cope with stress, both of which are well-established risk factors for heart disease. These habits collectively contribute to traditional heart disease risk factors, creating a vicious cycle where stress promotes unhealthy behaviors, which then exacerbate cardiovascular risk. Building sustainable, healthy routines is therefore a key aspect of stress management and heart protection.
Understanding ‘Broken Heart Syndrome’ and Other Effects of Stress on the Heart
One of the most striking demonstrations of the brain-heart axis is a condition often referred to as “broken heart syndrome,” medically known as Takotsubo cardiomyopathy or stress-induced cardiomyopathy. This unique condition occurs when sudden, intense emotional or physical stress, such as grief, anger, fear, or even extreme positive events, causes a rapid and severe weakening of the heart muscle. The symptoms can be alarming and often mimic those of a heart attack, including sudden chest pain and shortness of breath.
In Takotsubo cardiomyopathy, the left ventricle of the heart temporarily changes shape, often resembling a Japanese octopus trap (thus “Takotsubo”), leading to impaired pumping function. Crucially, this occurs without any blockages in the coronary arteries, which differentiates it from a typical heart attack. While usually temporary, with heart function typically recovering within a few weeks, it can be fatal in rare cases. Up to 30% of individuals who experience this syndrome are unaware of what triggered their symptoms, underscoring the subtle yet profound power of stress. This condition highlights the critical importance of emotional wellness as an integral part of a whole-istic health plan, as intense psychological distress can have direct and severe physical manifestations on the heart.
The Critical Link Between Stress, Sleep, and Heart Health
The intricate relationship between stress, sleep, and heart health forms a critical triad in our overall well-being. Stress is a notorious disruptor of sleep, often leading to insomnia or restless nights. The constant presence of stress hormones, particularly cortisol, can interfere with the body’s natural sleep-wake cycle, making it difficult to fall asleep and stay asleep.
Conversely, poor sleep itself acts as a significant stressor on the body. Chronic sleep deprivation can lead to elevated levels of stress hormones, creating a vicious cycle. Lack of adequate sleep has been consistently linked to higher blood pressure, increased inflammation, and impaired glucose metabolism, all of which are detrimental to cardiovascular health. It contributes to a higher risk of obesity and diabetes, further compounding the effects of stress on the heart. Prioritizing good sleep hygiene—ensuring a cool, dark, quiet sleep environment, avoiding screens before bed, and maintaining a consistent sleep schedule—is not just about feeling rested; it is an essential strategy for regulating stress hormones and protecting your heart from their long-term damaging effects.
Taking Control: A Whole-istic Approach to Protecting Your Heart from Stress
Taking proactive steps to manage stress is one of the most powerful ways we can protect our heart health and improve our overall quality of life. Embracing a whole-istic approach, one that nurtures the spirit, mind, and body, allows us to build resilience against the omnipresent pressures of modern living.
Lifestyle Strategies to Mitigate the Effects of Stress on the Heart
Effectively managing stress to protect your heart involves implementing a variety of lifestyle strategies that support your physical and mental well-being.
- Physical Activity: Regular physical activity is a potent antidote to stress. It helps reduce stress hormones like cortisol and adrenaline while stimulating the release of endorphins, natural mood elevators that promote a sense of well-being. Engaging in personalized fitness plans designed for your unique needs can significantly lower your blood pressure, improve cholesterol levels, and strengthen your heart. Activities such as general flexibility work and Pilates are excellent choices for active aging women, offering benefits for strength, balance, and stress reduction without high impact. To learn more about how we can tailor a fitness plan for you, explore our in-person training.
- Heart-Healthy Nutrition: The food we eat plays a vital role in our body’s ability to cope with stress and maintain cardiovascular health. Adopting principles of clean eating, focusing on whole, unprocessed foods, and being mindful of the glycemic index can stabilize blood sugar levels and reduce inflammatory responses. The heart-friendly Mediterranean diet, rich in fruits, vegetables, whole grains, lean proteins, and healthy fats, is an excellent example of an eating pattern that supports heart health and overall vitality. Adequate protein intake is also crucial for maintaining muscle and bone health as your body changes.
- Mindfulness Techniques: Incorporating mindfulness into your daily routine can significantly reduce stress. Practices such as deep breathing exercises and meditation help activate the parasympathetic nervous system, promoting relaxation and lowering heart rate and blood pressure. These techniques train your mind to respond more calmly to stressors, encouraging a sense of peace and comfort. Listen to music, read, call a friend, or get involved with special interest groups in your community. Explore impactful groups within your local church. Take time out for yourself to renew and replenish. If this task is challenging and you feel you need a little extra help, please reach out to a professional counselor. No shame in reaching out for help! It is important for our overall health.
- Quiet spaces and breath: Do you have a quiet place to meet yourself where you are? In the quiet spaces of prayer and mindfulness, we learn to listen not just with our ears but with our whole being, like Elijah on the mountain who discovered that God was not in the wind, the earthquake, or the fire, but in the gentle whisper (1 Kings 19:12). When we slow our breath, still our racing thoughts, and sit attentively before God, we make space for that soft, steady presence to be felt. Prayer becomes less about speaking and more about surrendering our noise, trusting that in the silence God is already speaking, guiding, comforting, and reminding us that we are never alone, even when the world feels loud. Try breathing patterns with focus and feel the difference!
- Social Connection: Building and nurturing a strong, supportive community is invaluable for stress management. Connecting with friends, family, or support groups provides emotional comfort and a sense of belonging, which can significantly buffer the impact of stress. Social interaction can reduce feelings of loneliness and isolation, which are themselves linked to increased cardiovascular risk.
When to Seek Help: Recognizing Symptoms and the Role of Medical Guidance
It is vital to recognize when the effects of stress on the heart may be signaling a need for medical attention. While stress management techniques are powerful, they are not a substitute for professional medical evaluation when symptoms are concerning.
Pay close attention to warning signs such as:
- Chest pain or pressure: Especially if it is new, severe, or radiates to your arm, back, neck, jaw, or stomach.
- Heart palpitations: A sensation of a racing, pounding, or fluttering heart, particularly if accompanied by dizziness or shortness of breath.
- Unexplained shortness of breath: Especially during light activity or at rest.
- Dizziness or lightheadedness: Which could indicate issues with blood flow to the brain or heart.
- Progressive or unusual fatigue: Beyond what is expected from your activity level.
If you experience any of these severe symptoms, particularly sudden chest pain, it is crucial to call 911 immediately. For persistent or concerning symptoms that you believe are stress-related, consulting a healthcare provider is the essential next step. They can assess your individual situation, rule out other conditions, and provide personalized guidance. Regular cardiac screening, including blood pressure measurements and cholesterol checks, is an important part of routine healthcare, especially as your body changes or if you are experiencing prolonged stress. Partnering with a specialist who understands the unique needs of women as they age can help you create a safe and effective wellness plan custom to your body’s changing requirements. Explore our virtual training options to receive expert guidance from the comfort of your home.
Frequently Asked Questions about Stress and Heart Health
Understanding the nuances of how stress impacts our cardiovascular system is key to proactive health management.
Can a single stressful event cause a heart attack?
Yes, in certain circumstances, a sudden, severe stressor can trigger an acute cardiac event, including a heart attack. While the direct cause of a heart attack is typically a blockage in a coronary artery, intense acute stress can act as a catalyst. A surge of adrenaline can increase heart rate and blood pressure, potentially causing a vulnerable plaque (a fatty deposit within the artery wall) to rupture. This rupture can lead to the rapid formation of a blood clot that completely blocks blood flow to a portion of the heart muscle. Additionally, acute stress can sometimes induce coronary artery spasm, temporarily narrowing the artery and restricting blood flow. These acute effects of stress on the heart are more likely to occur in individuals who already have underlying heart disease or pre-existing plaque buildup.
What are the first signs of stress-related heart problems?
The first signs of stress-related heart problems can often be subtle and easily dismissed, making them particularly dangerous. Many serious conditions, such as high blood pressure and high cholesterol, may have few or no obvious symptoms. However, some common indicators of stress impacting your heart include noticeable heart palpitations or fluttering sensations in your chest, consistently high blood pressure readings, or atypical chest discomfort that may not feel like typical “heart attack” pain. You might also experience unexplained shortness of breath during activities that were previously easy, or a persistent, unusual fatigue. It is important to listen to your body and not dismiss these signs as merely “stress” or “aging”; they warrant a conversation with a healthcare professional.
Can you reverse the effects of stress on your heart?
While some structural damage from events like a heart attack is permanent, many of the negative effects of stress on the heart can be managed, improved, or even reversed through dedicated lifestyle changes. Stress itself is a modifiable risk factor. By consistently engaging in regular exercise, adopting balanced nutrition based on clean eating principles, prioritizing quality sleep, and implementing effective stress management techniques, you can significantly reduce inflammation, improve blood pressure, stabilize blood sugar and cholesterol levels, and improve overall cardiovascular function. This whole-istic approach can help mitigate the progression of heart disease and foster a more resilient cardiovascular system, even as your body changes. It’s about empowering your body’s natural healing capabilities and building a foundation for long-term well-being.
Conclusion: Building a Heart-Healthy Future
The journey to understanding and mitigating the effects of stress on the heart is a powerful step towards a healthier you. Making certain to have regular checkups with your healthcare provider is an important step. Understanding how both acute and chronic stress can directly impact your cardiovascular system through hormonal surges and inflammatory responses, as well as indirectly through unhealthy coping behaviors, is crucial for maintaining your overall health. We have also highlighted unique conditions like “broken heart syndrome” and the critical link between stress, sleep, and heart health. Learn and research as much as you can to advocate for your health. Hire a fitness trainer or health coach to help you develop healthier habits.
The good news is that stress is a modifiable risk factor, and you have the power to influence its impact on your heart. By embracing a proactive, whole-istic approach that prioritizes physical activity, heart-healthy nutrition, mindfulness, and strong social connections, you can build remarkable resilience. Our commitment at Personalized Fitness For You is to nurture your spirit, mind, and body, guiding you through personalized fitness plans and wellness strategies designed to support your personalized needs! We believe in meeting individuals where they are and building beyond. Located in the Winona Lake and Warsaw area, offering in-studio sessions as well as meeting people in the US virtually!
The effects of stress on the heart don’t have to define your future. Take a proactive step towards whole-istic wellness today. Contact Joy today to schedule your complimentary consultation with Joy, owner & certified trainer, and begin your customized fitness journey in Warsaw, Indiana. If you don’t live in the vicinity for training, no problem, consider meeting virtually.